Way back in 2010, I decided to do the AIDS walk with my high school classmates. I ended up walking six miles, and felt proud of that. Later, though, when I got home and all the activity had ended, I was incredibly sore and my legs ached all over. A few days after that, I was walking home with a friend when my left leg began to drag across the sidewalk. “I can’t lift my leg,” I told her.
I tried to put on a brave face in the day or two that followed while in school, but the pain was enough for me to make a call to my mom during class and ask to be taken to urgent care at the same hospital where I’d been a patient. Since I almost never complained about pain, I was taken to the hospital promptly. I waited there for a while, and eventually got an MRI of my hip.
Days after that I met with my surgeon. He’d performed all my surgeries and had known me since I was a baby. “You have tendonitis,” he told me. “The muscle is inflamed.”
I reminded him that I walked the AIDS walk, and in my naivete I thought he’d say something about how proud he was of me for contributing to such a great cause.
Instead, he looked at me and said, “Don’t do it again. It isn’t worth it. Bottom line, you shouldn’t be in pain.”
It’s no secret that I am a product of the medical system and always have been. I didn’t quite feel that way when I was younger, though…probably because I was too young to realize it. I didn’t have the level of self-awareness that I feel I have now. I hadn’t yet grasped the complexities of such a truth…that I’ve been, essentially, a medical object because of my diagnosis.
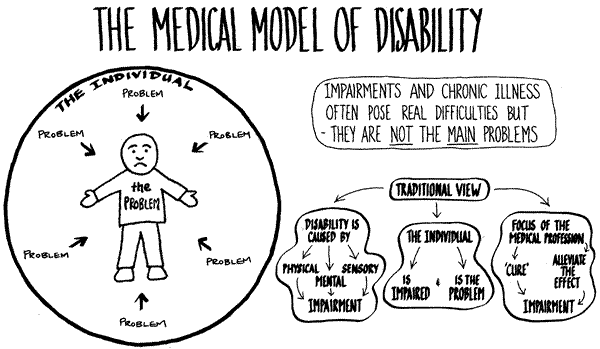
It got me to thinking about the medical model of disability. My understanding of this model is that it defines disability as an intrinsic part of the individual, which may reduce the person’s quality of life or cause the person some disadvantages. According to this model, managing a disability involves identifying it, understanding it, and then trying to control it or alter its course.
A part of me subscribed to this model for some time, probably because I am such a realist. That is, I do have a disability and I definitely needed medical intervention to manage it and to obtain a better quality of life. However, this notion that a diagnosis needs to be “cured” in order for bodies to be deemed acceptable is a concept I do not agree with. Cerebral palsy has no cure, but I feel that my body is as acceptable as that of a non-disabled person. The question of whether or not I would accept a cure if there were one is an entirely different conversation, and one that I often consider a waste of time.
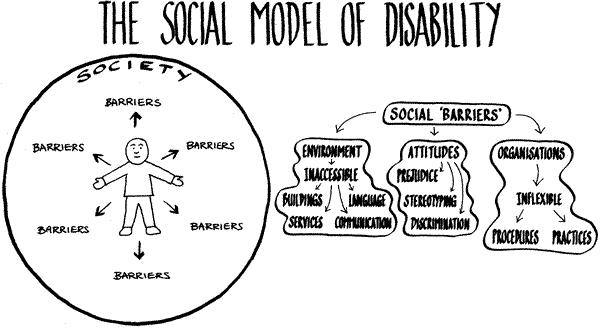
I think I lean more towards the social model of disability, by contrast. This model emerged from the World Health Organization (WHO), and examines the social aspects of living with a disability, like accessibility, accommodations, and equity. This new paradigm strives to provide an individual with a disability access through accommodations and inclusion. Additionally, this model attempts to remove several physical, cultural, and educational barriers that may be present.
That being said, this idea that my own body should be limited or controlled by anyone other than me is flawed. For example, the fact that I was reprimanded for participating in the AIDS walk instead of supported–by someone I idolized, no less–didn’t feel right. The tensions between the autonomy of my body and being embedded in this medical system are ever present. I don’t necessarily mean that my identity is only that of a patient, but rather that it goes far beyond that label. I am more than my diagnosis and I always will be, even when my physical limitations try and stop me. A big part of my identity includes solidifying who I am in society and how I can contribute in a positive way.

You my dear never seem to disappoint!!!!❤️
LikeLike